You rested.
You did your clamshells.
You completed physiotherapy.
But when you returned to running along the Don Valley Trail or lifting at your downtown Toronto gym… the pain came back.
If you’ve experienced a gluteus medius or gluteus maximus tear, you’re not alone. Many people take weeks—or even months—off to recover, only to notice persistent discomfort, weakness, or instability when they resume activity.
As a Toronto chiropractor specializing in NeuroStructural Corrective Care, I often see patients who are told their muscle has “healed,” yet something still feels off.
Let’s explore why.
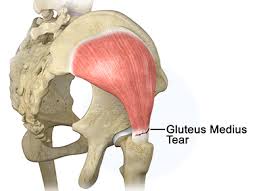
Understanding a Glute Tear
The Gluteus medius and Gluteus maximus are essential for:
The glute medius stabilizes your pelvis during gait.
The glute maximus powers hip extension and protects your low back.
When either muscle tears—whether partially or more significantly—rest and graded strengthening are necessary. According to guidance summarized by the Canadian Chiropractic Association, proper musculoskeletal rehabilitation involves restoring strength and functional movement patterns.
But here’s the missing piece:
Healing tissue is not the same as restored function.
The Common Recovery Trap
Many people take significant time off activity after a tear. The inflammation settles. The muscle fibers repair.
Yet when they return to sport, they notice:
Why?
Because recovery often focuses on the injured muscle alone—without examining the spine alignment and nerve supply controlling that muscle.
The Overlooked Root Cause: Low Back Dysfunction
Your glutes don’t operate independently. They are neurologically driven by nerves that exit the lumbar spine.
If there is dysfunction in the lower back—such as joint restriction, pelvic misalignment, or mechanical nerve irritation—it can lead to nerve inhibition of the glutes.
That means:
Your brain is not fully activating the muscle.
At my Downtown Toronto clinic, I frequently assess patients who demonstrate:
If nerve signaling is disrupted, even subtly, your glutes may not fire properly. Over time, this can:
This phenomenon is sometimes referred to as arthrogenic muscle inhibition—where joint dysfunction alters muscle activation patterns. While research is ongoing, current evidence suggests spinal and joint dysfunction can influence neuromuscular control patterns.
In simple terms:
If the wiring isn’t optimal, the muscle won’t perform optimally.
Another Possibility: Underactive → Then Overloaded
Not every tear happens because a muscle was “working too hard.”
In many cases, the glute was underactive for months or years.
Common Toronto lifestyle factors:
When a glute is chronically under-recruited, other muscles compensate.
Then one day:
Suddenly, the glute is required to generate force it hasn’t been conditioned for.
That mismatch between demand and readiness increases injury risk.
After healing, if activation patterns haven’t been restored, returning to activity recreates the same imbalance.
Why Strength Alone Isn’t Enough
Traditional Rehabilitation often emphasizes:
These are valuable. But here’s the critical distinction:
Strength does not equal activation.
You can have a muscle that tests strong in isolation but fails to fire efficiently during real movement—like walking, running, or squatting.
Effective recovery requires:
Without these components, the muscle may fatigue quickly or shift load to the low back.
The NeuroStructural Corrective Approach
At Dr. Mateusz Krekora Chiropractic Clinic, we look beyond the torn tissue.
Our NeuroStructural Corrective Process focuses on:
1. Lumbar Spine Assessment
We evaluate joint motion in the lower back to identify dysfunction contributing to nerve inhibition.
2. Pelvic Alignment
Subtle imbalances in the pelvis can alter glute recruitment patterns.
3. Neurological Activation Testing
We assess how well your glutes activate during movement—not just at rest.
4. Corrective Adjustments
Precise chiropractic adjustments aim to restore joint mobility and reduce mechanical nerve irritation.
The Ontario Chiropractic Association notes chiropractic care is commonly used for managing mechanical low back dysfunction—an area closely tied to glute activation.
When spinal mechanics improve, many patients notice:
What Hope Looks Like After a Glute Tear
If you’re frustrated because:
There is hope.
Recovery involves more than rest and clamshells.
It involves:
When those pieces align, patients often return to running, lifting, cycling, and hiking stronger than before.
Practical Recovery Tips for Toronto Patients
While undergoing corrective care, I often recommend:
-Gradual Load Progression
Avoid jumping back into previous intensity levels too quickly.
-Single-Leg Stability Drills
Focus on control, not speed.
-Core + Pelvic Integration
Dead bugs, bird dogs, and controlled step-downs can support glute re-education.
-Monitor Low Back Symptoms
Recurring stiffness may indicate unresolved lumbar dysfunction.
Feel Strong, Live to the Fullest
A glute tear can feel like a major setback—but it doesn’t have to define your long-term mobility.
If your muscle has healed but you’re still struggling, it may be time to look deeper.
At Dr. Mateusz Krekora Chiropractic Clinic in Downtown Toronto, we focus on correcting the root cause—not just treating the injured tissue.
Because true recovery means:
Ready to feel like you’re 25 again?
👉 Book Your Free Case Review and let’s uncover what’s really holding you back.
This article is for informational purposes only and should not be taken as medical advice. Please consult a licensed chiropractor before starting any treatment.
